The mission of the Center for Computer Integrated Surgical Systems and Technology (CISST ERC) is to develop computer-integrated surgical (CIS) systems that will significantly change the way surgical procedures are carried out. Specifically, we will develop a family of systems that will combine innovative algorithms, robotic devices, imaging systems, sensors, and human-machine interfaces to work cooperatively with surgeons in the planning and execution of surgical procedures. Our goal is to produce systems that will greatly reduce costs, improve clinical outcomes, and increase the efficiency of health care delivery. By improving therapeutic precision and consistency, these systems will reduce therapeutic risks and enable the development of new treatment options.
We are addressing key knowledge, technology, and system design challenges that must be overcome in the development of CIS systems. By working closely with industry and clinicians, we will promote transfer of these results into clinical use and help educate a new generation of engineers, clinicians, and researchers needed to support this rapidly expanding field.
Systems Vision – Coupling Information Technology to Surgical Actions to Significantly Change Surgery
The growing demand for complex and minimally invasive surgical interventions is driving the search for ways to use computer-based information technology as a link between the preoperative plan and the tools utilized by the surgeon. Figure A-1 illustrates the architecture of CIS systems. At the core is a computer or network of computers performing modeling and analysis tasks such as image processing, surgical planning, monitoring and control of surgical processes. A variety of interface devices permit the computers to obtain images and other information about the patient, to assist physically in the surgical intervention, and to communicate with the surgeon and operating room personnel. The computers have access to anatomical atlases and statistical databases that can be used to assist in surgical planning, execution, and follow-up.
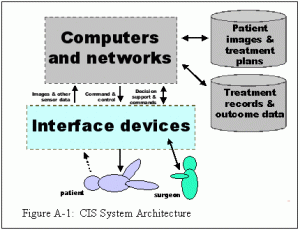
Data flow associated with these systems is illustrated in Figure A-2. Images and other information about a patient are combined with statistical atlases of anatomy to create a patient-specific model for use in surgical planning. In the operating room, imaging and other sensing is used to register the preoperative model to current reality and to update the model and plan. Once this is done, the surgeon may supervise a robot that carries out a specific treatment step, such as inserting a needle or machining bone. In other cases, the CIS system will provide information to assist the surgeon’s manual execution of a task, for example through the use of computer graphic overlays on the surgeon’s field of view. In yet other cases, these modes will be combined. Post-operatively, the same imaging, modeling, and analysis capabilities can be used to facilitate patient follow-up and longer-term assessment of the effectiveness of treatment plans.
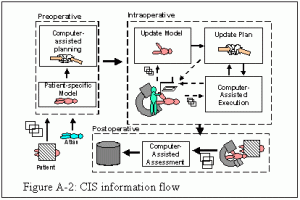
We refer to this paradigm of patient-specific modeling and planning, coupled with computer-assisted surgical execution and follow-up, as Surgical CAD/CAM, emphasizing the analogy with computer-integrated design and manufacturing systems. We refer to these CIS systems that work interactively with surgeons to extend human capabilities in carrying out surgical tasks as Surgical Assistants. These characterizations are complementary and not mutually exclusive. They draw upon common technologies, and real systems often have both CAD/CAM and Assistant traits. Nevertheless, the terms are useful as a means of structuring our vision of CISST.